Cutting the carbon out of concrete
The Radical Ceramic Research Group is pioneering potentially transformative alternatives to traditional concrete, the world’s second largest source of emissions.

Common neurological disorders like depression and chronic pain can be challenging to treat with conventional methods. An automated version of a long-used brain stimulation technique holds real promise as a reliable and effective drug-free alternative.
When he talks about the brain, Risto Ilmoniemi has a striking habit: he tends to point at his own. So, as he describes the relationship between the right and left hemisphere or the workings of the motor cortex, the Aalto University professor gestures at specific locations on the surface of his head.

Most people tend not to think about their brain regions as they navigate the world, but Ilmoniemi clearly does. It’s humbling when you stop to consider it: all of human experience is mediated by approximately 1300–1400 g of tissue inside our skulls. As you read these words, somewhere at the back of your head, the visual cortex is active, and as you scroll down with a finger or thumb, the motor neurons near the top of your head are firing away.
Ilmoniemi has spent most of his career thinking about this neurological geography. In particular, he’s interested in ways the brain’s operations might be enhanced through technology: fixing glitches, correcting flaws and intervening when it’s failing.
Ilmoniemi and his colleagues in the ConnectToBrain project — a collaboration between Aalto University, University of Chieti-Pescara in Italy and University of Tübingen in Germany — are world-leaders in the science of transcranial magnetic stimulation (TMS). Using magnetic coils positioned adjacent to the skull, TMS involves non-invasively zapping pulses into the head to induce electric fields within brain tissue that promote or dampen neurological activity.
When doctors apply these pulses in clinics, TMS can effectively treat pain, severe depression and many other conditions. ‘If you stimulate many times at the same region or same spot, the brain will change,’ says Ilmoniemi. And remarkably, the effect can persist. For many conditions, drug treatment hasn’t worked or is undesirable, so TMS offers a powerful alternative.
However, TMS is still in its infancy as a treatment. At the moment, the technique requires expert human operators. It’s time-consuming, therefore expensive, and so far the stimulation patterns tend to be relatively simple.
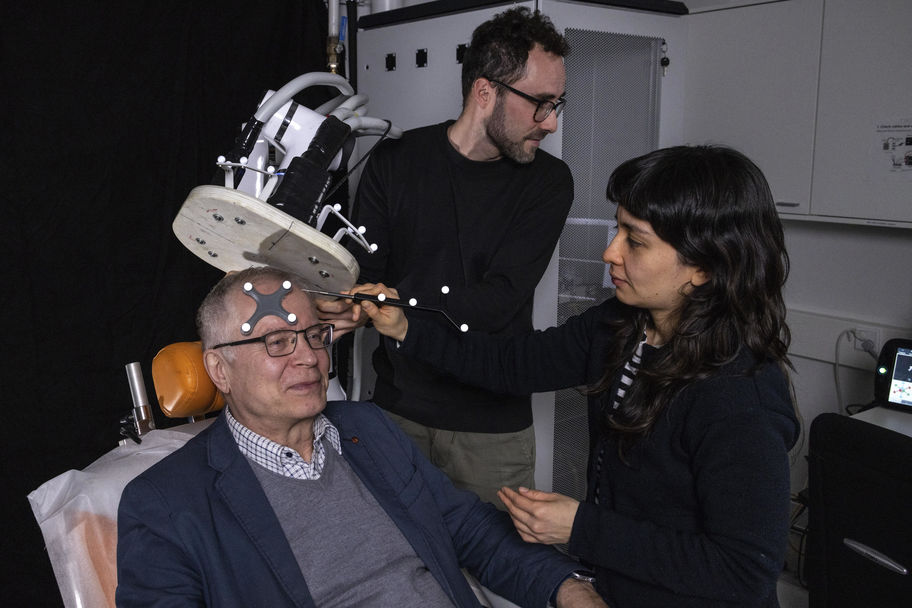
That’s why Ilmoniemi and his colleagues are building a new generation of devices that can stimulate brain networks at multiple places simultaneously or at short intervals. The technology is underpinned by smart algorithms that can listen and respond to the brain’s activity on the fly. Not only could this improve the efficacy of existing TMS treatment, but it might enable entirely new stimulation patterns that could treat myriad other conditions. And since expert human operators are not required, TMS could be introduced more widely into hospitals and clinics.
Ilmoniemi imagines a future where TMS is deployed worldwide – perhaps even in people’s homes – and where intelligent algorithms help scientists and doctors identify new beneficial sequences for stimulating the brain, opening up as yet unidentified avenues for treatment.
‘That's the dream. That's what we hope,’ he says.

TMS has come far since its first experimental tests in the 1980s. When researchers in the UK started applying magnetic coils to people’s brains, they were essentially guessing where to place them: for instance, hoping to stimulate motor neurons somewhere beneath the skull.
Around the turn of the 21st century, more advanced TMS technology began to be used in conjunction with MRI scans, allowing the pulses to be targeted much more precisely.
Since then, hundreds of studies have explored the efficacy of TMS for a variety of conditions. Some of the most promising studies have been in patients with severe depression, neurological pain, multiple sclerosis, fibromyalgia, Parkinson’s disease or stroke. There’s also evidence for potentially treating conditions such as schizophrenia, obsessive compulsive disorder, addiction and post-traumatic stress disorder. New possibilities are emerging every year. For example, if researchers can work out the correct regions and sequences to target, TMS might eventually help slow the onset of memory loss in patients with Alzheimer’s disease.
While TMS’s usage varies between countries because of differing legal and regulatory rules, it’s now more accessible to patients than ever before – and the scope of the treatment as an alternative to drugs, or a complement to other therapies, is growing.
Selja Vaalto, a specialist in clinical neurophysiology at Helsinki University Hospital, uses TMS to treat people suffering from neuropathic pain, such as patients who have experienced brain damage after a stroke, or more unusual cases like phantom limb syndrome, where people report feeling pain in an arm and leg after it has been amputated.
‘These are patients where nothing else has helped them,’ Vaalto explains. For neuropathic pain, drug relief often doesn’t work. On questionnaires, many of these people report their pain as a 10 on a scale of 1–10, she says, so intervention with TMS can be transformative in reducing their discomfort, supporting sleep and alleviating what can sometimes be agony without respite.
As Vaalto explains, a patient starts the TMS treatment process by visiting the clinic once a day for two weeks. Doctors place a wand on the surface of their skull – developed by the spin-off company Nexstim founded by Ilmoniemi – for 15 minutes. Every second, 10 pulses are fired, zapping the brain regions thought to be related to pain. In the first week, the target is in the motor cortex; if that doesn’t relieve pain, the focus turns to the secondary somatosensory cortex.

Elsewhere in the hospital, another team uses TMS for alleviating depression – another condition where it can be helpful to offer patients an alternative to drugs. And Vaalto also helps surgeons prepare for operations on brain tumours or epilepsy interventions by identifying areas they need to protect while operating. ‘We can make a map for the neurosurgeons and show them the important areas,’ she says. For example, TMS coils can be used to provoke indicative hand, face or leg twitches in the motor cortex or to identify the most important regions for speech by temporarily preventing people from talking clearly.
However, Vaalto is well aware that these commercial devices are basic compared with prototypes in the laboratory. As a member of the ConnectToBrain team, she works away from the hospital one day each week, helping in the design of the next generation of this technology.
Most current commercial TMS devices have only one coil within the wand. ‘With commercial devices, you cannot adapt to changes in the brain,’ explains Victor Souza of the ConnectToBrain team. ‘If you want to, let’s say, “play together” with the brainwaves, you cannot, because you need to move – by hand – the stimulator to a different location.’

Souza, Vaalto, Ilmoniemi and their colleagues are working to change this. Their idea? Embed multiple coils of different shapes within the same device: figures of eight, loops and circles, which allow for much more intricate and flexible control.
They started in 2017 with a simple device that had two coils superimposed over one another.
But more recently their coils have gotten more complex, with the latest device housing five different shapes.
The next step is to build a device that spans across the surface of the skull. ‘We want to expand it to the whole brain. Many brain functions come from the communication of different areas: the frontal part does something, the back of the brain does another thing and so on. So we want to be able to reach all of them fast,’ says Souza.
Adding robotic control and machine learning algorithms to the mix creates even more possibilities. With all these technologies combined, researchers could identify entirely new ways to stimulate the brain.
As the ConnectToBrain team’s multi-coil technology develops, underpinned by artificial intelligence, Ilmoniemi anticipates new avenues for brain stimulation and medical treatment.
To date, there have been thousands of TMS studies conducted around the world, but almost all have used single coils pointed at single brain regions by a human operator. Ilmoniemi believes that new patterns and sequences could be waiting to be discovered by stimulating the brain at multiple points and using algorithms that can learn.
‘One can think about the brain in many ways. One way is as a dynamical system with interacting parts,’ he explains. ‘Of course, there are neurons, but there are also nodes: collections of neurons in different parts of the brain that have different functions, producing a network.’

Depression, for instance, does not emerge from a single location in the brain but rather through the interaction of many nodes: a network. Therefore, treating the brain more effectively with TMS may require more complex stimulation patterns spanning different regions in the brain.
Another promising avenue that the ConnectToBrain team is exploring for future TMS treatment is to respond to the overall brain state.
This could start simply. ‘We know now that the neurons in the brain are working in an oscillatory way,’ says Vaalto. If the TMS pulses could be targeted to certain phases of the oscillations, responsively and in real time, it could make the treatment even more effective. ‘I think that’s something that can be taken to the clinic in the near future,’ she says.
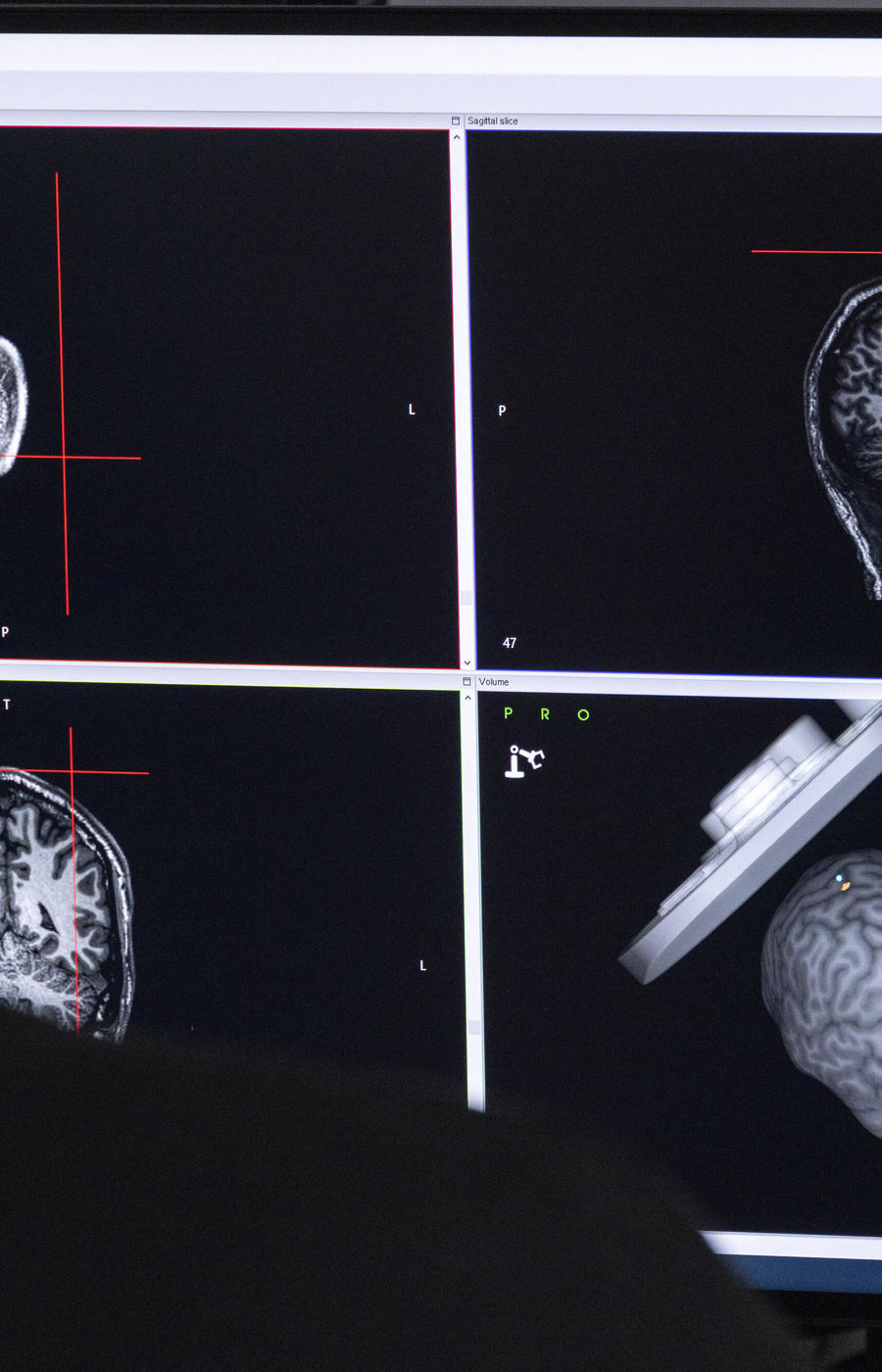
But in principle, responding to brain state could go further. Depending on what you're doing, resting or doing motor tasks or using language, the networks will act differently,’ says Ilmoniemi. This raises a hypothesis: if people were encouraged to perform different tasks during TMS sessions – say watching a video, or saying words out loud – would it change the efficacy of the treatment? Scientists don’t yet know for sure, but it’s exciting to contemplate.
Ilmoniemi compares it to playing jazz. It’s about working with the orchestra of the brain: after all, a good musician doesn’t play over the other instruments without listening; they seek to perform in harmony. Thus, when stimulating the brain, algorithms must base their targeting and timing on its rhythms and state.
Over the course of his career, Ilmoniemi has become fascinated by the possibilities of finding beauty in scientific discovery. Usually, beauty in science is reserved for elegant mathematics or awe-inspiring physics, but the professor also sees it in the brain – and in the technology of TMS.
‘I'm really motivated to try to understand the world mainly from the physics point of view: how the brain works, how it's related to what we experience, the experience of beauty, this mystery of consciousness. That's motivating me. And it's great to be working in an environment where other people are also interested in similar things,’ he says.
After all, Ilmoniemi and his team are seeking to improve the workings of one of the most complex objects known in the universe. While their endeavour may be technological and neurological, there’s undeniably art to it. We don’t yet fully understand the brain, and certainly not how it mediates the complexity of human experience, but the answers will come from within it, from inside that mass of grey and white matter. As Ilmoniemi points out, there’s beauty in those thoughts.

Text: Richard Fisher
Photos from the laboratory: Mikko Raskinen
* Dr. Baran Aydogan and Dr. Victor Souza have developed a method called tractrography to study cortical connections
Other images: Research group
Video: Anna Berg
Original 1985 paper on TMS
https://www.sciencedirect.com/science/article/pii/S0140673685924134
Review of conditions that TMS has efficacy for (2018)
https://pubmed.ncbi.nlm.nih.gov/31901449/
ConnectToBrain Multi-coil papers 2018, 2021 and 2022
https://www.sciencedirect.com/science/article/pii/S1935861X18300974
https://iopscience.iop.org/article/10.1088/1741-2552/ac3207
https://www.sciencedirect.com/science/article/pii/S1935861X21008299
https://www.sciencedirect.com/science/article/pii/S1935861X22000213

Translating research findings into clinical patient care is a long process that builds on previous scientific advancements. Donate and support the development of medical technology for the well-being of us all.
Read about radically creative approaches that are turning fundamental research into tools to create a better future for us all.

The Radical Ceramic Research Group is pioneering potentially transformative alternatives to traditional concrete, the world’s second largest source of emissions.

A hyperspectral snapshot captures all the light in a scene, not just colours or infrared light. The extra information is useful in many applications, from agriculture and conservation to forensics and food safety.

Focusing on short-term profit isn’t sustainable. So what can we do to move in the right direction?
Antimicrobial resistance is causing a silent, stealthy pandemic – and the pipeline of new antibiotics is dwindling. The good news is that researchers are turning to other ways to fight bacteria, by targeting the very weapons they deploy during an infection.