The usability of electronic health record systems did not improve in four years

Usability focused questionnaires conducted in 2014 and 2010 are a part of the first national eHealth monitoring study on the usability and user experiences of electronic health record systems. In total, over 3 000 physicians actively doing clinical work responded to both questionnaires.
'There has been no improvement in the overall experience in four years even though the usability problems related to electronic health record systems were already known in 2010. The average school grade given to the systems by the physicians was 6–7, at an adequate level', explains Johanna Kaipio, a researcher at the Aalto University Department of Computer Science.
The respondents were experienced in using the electronic health record systems and the results of the study represent their experiences of the use and usability of these information systems.
Better grades in private sector
The physicians employed by healthcare centres and hospitals generally gave worse grades to the electronic health record systems they used compared to their colleagues working in the private sector. In fact, some brands received even worse grades in 2014 than in 2010.
'Kanta (the national archive of health information) and eResepti (electronic prescription) have not succeeded in making the work of physicians easier, and the collaboration and exchange of information between physicians working in different organisations, let alone between the physician and patients, still does not work as desired. On the other hand, the study highlighted functionalities where development has occurred. Among others, these include the support of information systems in preventing errors associated with medications, clarity of the patient's medication list and a summary view of the patient's health status,’ describes Kaipio.
Based on the research findings, the use of electronic health record systems does not yet support or enhance performing routine tasks by physicians in the desired manner. There is a need for development work to accomplish the benefits expected of the use of clinical information systems and support patient safety.
'The implementation phase provides an opportunity to have an influence on the ways that the clinical information system or its version are used and affect the changes in work processes enabled by the information systems. At this stage, it is important to also recognise possible shortcomings related to usability. Healthcare professionals must be supported in the transition and changes must be planned. These perspectives will be taken into account in the recently launched COPE project, which investigates how healthcare professionals can be supported in the adoption of eHealth services', Kaipio adds in the end.
The study was recently published in the International Journal of Medical Informatics. A number of articles related to the studies conducted in 2010 and 2014 have also been published in the Finnish Medical Journal (Lääkärilehti). In addition to the Aalto University Department of Computer Science, the Finnish Medical Association, the University of Helsinki and The Hospital District of Helsinki and Uusimaa, the National Institute for Health and Welfare, the University of Turku, the University of Oulu, and the University of Victoria in Canada were involved in the study. The study surveying physicians' user experiences on usability of their electronic health record systems will be repeated in 2017.
More information:
Johanna Kaipio
Researcher
Department of Computer Science
johanna.kaipio@aalto.fi
+358 50 593 6822
Read more news
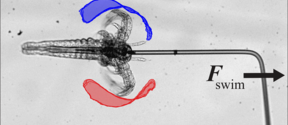
‘Mesoscale’ swimmers could pave way for drug delivery robots inside the body
Researchers have discovered how tiny organisms break the laws of physics to swim faster — such secrets of mesoscale physics and fluid dynamics can offer entirely new pathways for engineering and medicine.
Hanaholmen’s 50th anniversary exhibition lives on online – making the history of Finnish–Swedish cooperation accessible worldwide
MeMo Institute at Aalto University has produced a virtual 3D version of the anniversary exhibition of Hanaholmen.
Research reveals the economic significance of family firms in Finland
The findings show that, on average, family firms are more profitable and financially resilient than other firms – and also invest more.






